Pandemic Anxiety and the BDNF Gene in the Age of Coronavirus
- Home
- Blog

Biohacking Your Mental Health Ecosystem: Part One
“The world thus appears as a complicated tissue of events, in which connections of different kinds alternate or overlap or combine to determine the texture of the whole”
– Werner Heisenberg
My Dear Reader: could there be a relationship between Coronavirus and mental health? Other than the obvious connection between COVID-19 and our pandemic levels of social anxiety, is there more to it? From bat reservoirs; to wet markets selling wolf cubs, snakes, turtles, guinea pigs, rats, otters, badgers and civets; to humans circling the globe on airplanes and ships; the spread of this virus highlights a vastly interconnected ecosystem that applies as much to pandemics as it does (as you will soon learn) to your own mental health.
Our global ecosystem seems ever more interrelated, and perhaps ever more fragile and needing our protection, doesn’t it? From global warming, to global economic system correlations, to global pandemics, to global Internet connectivity, we live in an increasingly networked and interconnected world.
Coping with Pandemic Anxiety in an Uncertain World
In the past two years, I have taken you on three separate journeys that I hope have enlightened and inspired you, and helped you and your loved ones better understand your mental health and how to heal it. Through our series on genetic testing and the microbiome—“DNA: I Am Who I Am… or Am I?”, “DNA: Nurture Your Nature”, and “Your Mighty Moody Microbiome”—we have explored many of the underlying cellular building blocks that affect one’s mood, anxiety, cognitive functioning, and overall wellbeing. We also covered what to do when your condition is “treatment resistant,” and how to determine the reasons why (and how to treat them) under the Biopsychosocial Model.
A good summary of these blogs can be found in posts about “Your Mental Health Genes” and “Your Brain Health Genes.”
Along the way, we introduced you to the emerging field of Genetic Testing and how it influences our understanding and treatment of depression, bipolar disorder, PTSD, OCD, ADHD, and other conditions that bring about emotional pain and (at times) unremitting suffering, including pandemic anxiety.
Today, we embark on a new journey that I hope will bring you a sense of awe and wonder, as well as offer specific tools and tactics with respect to improving how you feel and function, and your overall quality-of-life. Today, we will begin to explore the profound, extraordinary, highly complex phenomenon known as “Your Mental Health Ecosystem.”
Biohacking Your Way to Improved Mental Health
Your mental health ecosystem is comprised of all of the genetic, biological, nutritional, microbial, interpersonal, unconscious, cultural, and spiritual factors that continuously interact and interrelate with one another from the moment you were conceived. This includes these elements of your “physical self”:
32 trillion cells, each cell comprised of…
- 100 trillion atoms
- 2 trillion molecules
- 25,000 protein-coding genes
100 trillion microbes inside your gut microbiome—an extraordinary manufacturing plant comprising…
- 1000 different species of bacteria
- Producing tens of thousands of previously unidentified proteins—critical building blocks that affect human health
- Producing millions of neurotransmitters, hormones, vitamins, and molecules that regulate the expression of your genes in every cell of your body
100 billion neurons in your brain…
- Connecting with one another across up to 1,000 trillion synapses
- Each one firing up to 450 times per second
- These cells and synapse process up to 400 billion bits per second of information
85 billion glial cells in your brain…
- Providing support and protection for neurons, including nutrients and oxygen
- Destroying bacteria, viruses, and toxins that threaten the brain
- Digesting and disposing dead brain cells
If you’re having a hard time wrapping your mind around those numbers inside the “physical you”, you’re not alone! To make things more concrete, here is a pictorial example of how a single gene, BDNF, lives in its own “complex ecosystem” inside your brain:
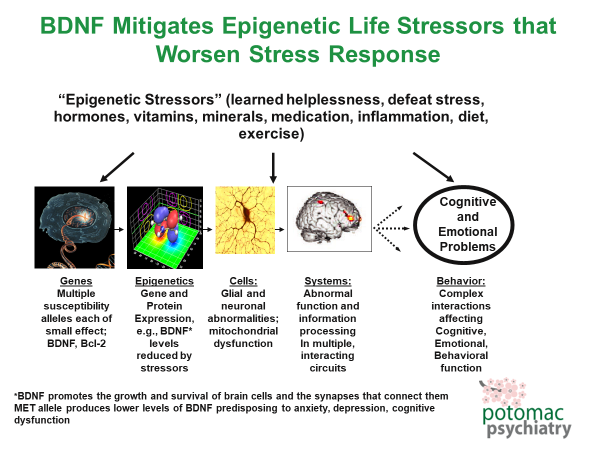
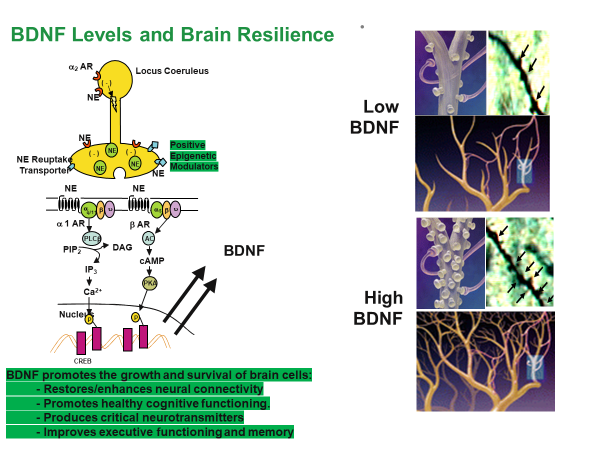
In the picture immediately above, the “Low BDNF” images depict relatively few neurotransmitters and dendrite branches when compared to the “High BDNF” images. Higher levels of neurotransmitters and dendrite branching promote more synaptic connections and better mental health. So how do we “biohack” our BDNF gene to increase its expression and strengthen our resilience to stress? The following picture provides you four ways to boost BDNF levels.
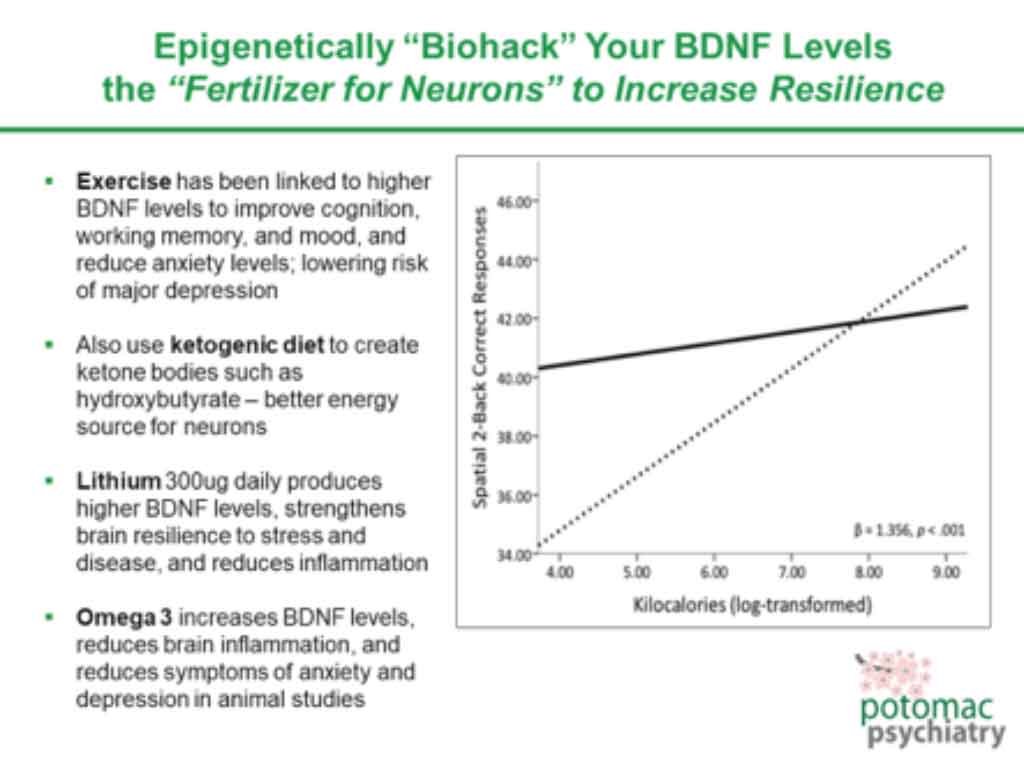 There is also research documenting that molecules like BDNF can also boost immune system function, and who wouldn’t like a stronger immune system in the Age of Coronavirus?
There is also research documenting that molecules like BDNF can also boost immune system function, and who wouldn’t like a stronger immune system in the Age of Coronavirus?
Limiting Our Pandemic Anxiety through Precision Medicine
WOW! We can biohack our BDNF gene to improve our emotional resilience, reduce pandemic anxiety, and boost our immunity! And this complexity relates to just one gene. How elegant and extraordinary is our human ecosystem?! And how does this complex system relate to your mental health?
Here’s the hook: for many patients, a thoughtful, systematic approach to understanding their entire ecosystem, including the forces and factors that affect these hundreds of trillions of cells, is absolutely essential to restore mental health. Why?
In our practice we evaluate and treat around 50 new patients per month, and 70-80% of these new patients have already received treatment from another psychiatrist—one patient had seen 13 different psychiatrists over several decades! The vast majority of these patients were treated under what is known as a “population-based” model of treatment. Our health-care system still generally operates as a one-size-fits-all model. This paradigm suggests that in the majority of people, a mental health problem – such as depression or bipolar disorder — has a common predicted trajectory, and most people will benefit from a homogeneous course of treatment. If a particular treatment does not work, then the second-most likely successful treatment plan is prescribed. This continues until the ailment is relieved. Treatments are based on available population statistics, and trial and error is used until the patient gets well. In this model of medicine, personal characteristics, risk factors, lifestyle choices and genetics are rarely considered.
There is an urgent need for what is known as “personalized medicine,” whereby each individual’s unique genetic, microbial, cellular, molecular, and interpersonal ecosystem is analyzed and systematically addressed toward better mental health. One needs to build a unique “personal mental health database” to create what we call a Personalized Precision Psychiatry approach. That’s what Potomac Psychiatry offers, and that’s what we’ll be exploring in the months to come on this blog.
To learn more about what this approach entails, read how we applied Personalized Precision Psychiatry to restore Adele’s Mental Health Ecosystem.
Telepsychiatry
And to learn more about how we are evaluating and treating pandemic anxiety in the Age of Coronavirus, using telehealth and telemedicine technologies, visit our Telepsychiatry landing page.
Be well, and please stay safe.
.png?width=144&height=144&name=Untitled%20design%20(34).png)



