Genes, Stress, Nutrition, and Antidepressants – How They Affect Anxiety, Depression, and Bipolar Disorder
- Home
- Blog

The brain is the organ of the mind. Our ability to think, feel, and experience life is dependent upon neurobiological processes governed by the interaction between our genes and various types of psychological, environmental, and physiologic influences and stressors. New research in the field of “epigenetics” offers compelling support for the combination of psychotherapy, nutrition, and medication management in the treatment of patients suffering from anxiety, depression, or bipolar disorder.Epigenetics means “over or above genetics,” and refers to how both the external environment and internal physiologic environment can interact with the DNA within the nucleus of each cell in the body, to alter how these cells function. In psychiatry, this field brings us knowledge regarding the epigenetic influences on brain cell function in patients suffering from mood disorders and anxiety. This knowledge carries profound implications for how we live our lives.
In mood and anxiety disorders, there is no “depression gene” or “anxiety gene.” One inherits a susceptibility to these conditions through multiple different genes, but the genes alone do not cause the illnesses. The genetic material within the nucleus of brain cells must first be influenced by epigenetic factors that come from outside the brain, such as external environmental or internal physiologic factors. Certain types of interpersonal stress with loved ones, or colleagues at work; inflammation, such as that caused by fat cells; and alcohol or drugs of abuse; can interact with these susceptibility genes to cause major depression or bipolar disorder; or cause anxiety disorders such as generalized anxiety, obsessive compulsive disorder (OCD), or panic disorder.
Two types of interpersonal stress can contribute to triggering psychiatric disorders. The first is called “learned helplessness,” defined as “a behavioral state of a person who believes that he or she is ineffectual, his or her responses are futile, and control over the environment has been lost.” The second is termed “social defeat stress,” and is defined as “relationships characterized by aggression, bullying, chronic subordination and humiliation.” Research has demonstrated that both learned helplessness and social defeat stress are epigenetic factors associated with psychiatric disorders.
Drugs of abuse such as cocaine trigger epigenetic changes in certain brain regions, affecting hundreds of genes at a time. Some of these changes remain long after cocaine has been cleared from the body. Research suggests that some of the long-term effects of drug abuse and addiction (including high rates of relapse) may be written into the epigenetic code (again, the interaction between the environment and the genes). Cocaine not only alters the epigenetic status of genes but also induces specific epigenetic modifications depending on how often the drug is used. Certain genes are switched on by infrequent administration, while others are switched on only after chronic administration (such as in addiction). Some are switched on by both This may relate to cocaine’s ability to “kindle” mood disordersAlcohol abuse has also been associated with epigenetic changes to the chromatin of the DNA in brain cells, predisposing to anxiety symptoms. And at a recent Society for Neuroscience meeting, marijuana use in teens was associated with cognitive deficits, reduced executive functioning (attention, focus and decision making), and changes in brain function in the frontal cortex. Whether marijuana asserts its effects through epigenetic mechanisms is the subject of ongoing research.
Obesity and nutritional aspects of a person’s lifestyle can also have profound effects on mood regulation and the onset of depression. We now know that fat cells release cytokine and C-reactive proteins. These proteins are known to cause inflammation throughout the body, and are associated with psychiatric disorders in the brain. They lead to alterations in neurotransmitter levels, neuroendocrine systems, and howbrain synapses function. This leads us to conclude that obesity is also a type of stressor that contributes directly to altered brain function associated with mood disorders – more specifically depression.
How do these multiple internal and external influences interact with the genetic material within our brain cells to initiate the onset of an emotional disorder? In the brain, an important function of the DNA that makes up our genes and chromosomes is to code messenger RNA, which in turn codes so-called neuroprotective proteins. These protective proteins, for example BDNF (Brain Derived Neurotrophic Factor), support and protect normal brain cell structure and function, and enhance memory, learning, higher order thinking, and neurogenesis – the growth of new brain cells which occurs throughout the lifespan.
Below is a picture of how depression and anxiety are triggered by the interaction between various types of stressors and the DNA found in every brain cell. As depicted from left to right, multiple different genes predispose the patient to developing depression or anxiety, as they are exposed to one or more of the stressors cited above. The genes are necessary but not sufficient to cause the illness by themselves. In response to the stressors, the genes are suppressed in their ability to manufacture the neuroprotective proteins such as BDNF; and Bcl-2, which prevents brain cell death. As the levels of these protective proteins drop, the brain cells begin to function abnormally; and the energy centers of the cells, the mitochondria, begin to malfunction as well. This in turn affects the function and structure of the brain cells that form information processing circuits, which then results in the changes in mood, behavior and thinking we see in those who suffer from depression, bipolar disorder, and anxiety.
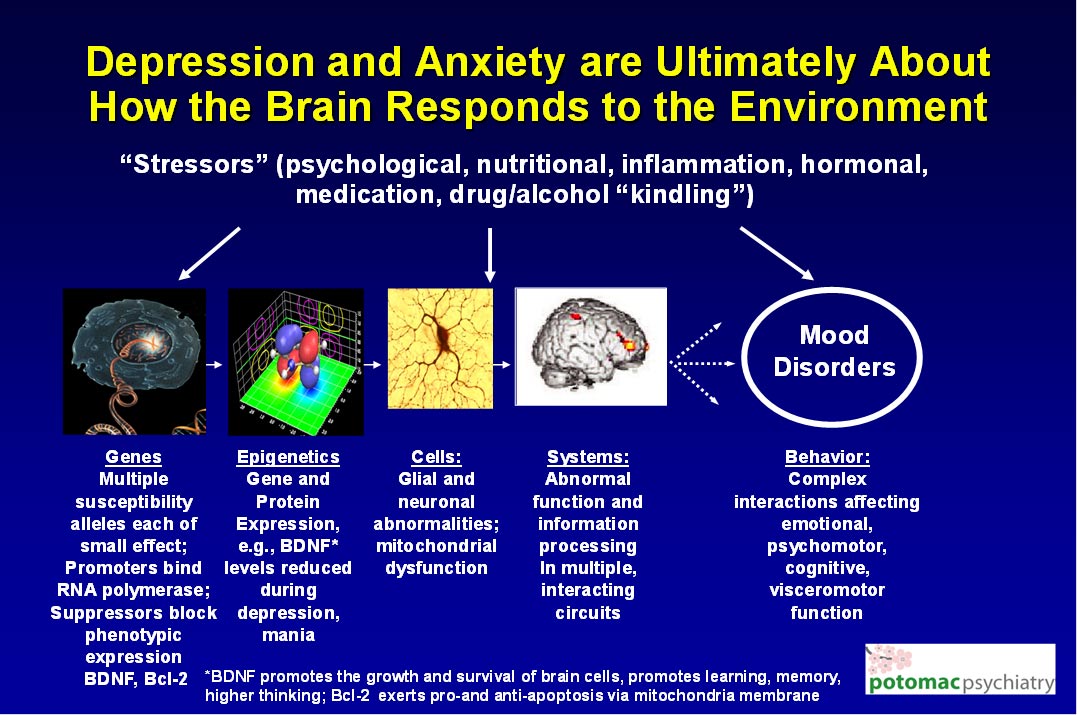
Neurogenesis is also critically important in the recovery from mood disorders, and can be positively affected by exercise, antidepressant medication, and through psychotherapy. Psychotherapy enables the patient to overcome the causes of learned helplessness and socially induced defeat-stress, characterized by repeated experiences of being overpowered and feeling helpless and trapped, whether in relationships at home or at work. Therapy empowers patients and enables them to leave behind destructive relationships from the past which have been internalized (for example damaging childhood experiences with a parent); and to modify or end current relationships that are characterized by repeated emotional battering. These emotionally damaging relationships may originate in one’s immediate or extended family, or in the workplace. In learning how to better manage or separate oneself from these types of stressful internal and external relationships, it can lead to increased resilience, new and richer social experiences, and result in neurogenesis.
Healthy nutrition can also play a key role in the recovery from a major mood or anxiety disorder. Reducing one’s body fat percentage to reasonable levels, for example 21% to 24% for women, and 13% to 17% for men, will reduce the release of the inflammatory proteins from fat cells. This not only has a salutary effect on brain cell function, but also reduces the likelihood of developing Type 2 Diabetes, coronary artery disease, hypertension, and stroke. Diets rich in lean protein, such as chicken, fish, egg whites, turkey, and whey protein shakes blended with fresh or frozen fruit; and filled with low glycemic index carbohydrates, such as fresh fruits and vegetables; with the use of olive oil (and not other vegetable oils or butter); combined with aerobic exercise three to four times per week; can assist in achieving these important goals of reducing body fat percentages. A sustainable program with proven success in accomplishing these objectives is The Joe Dillon Difference. Joe Dillon has coached many business executives, professionals and their families, in addition to 22 Olympic medalists who have won 60 medals, in a lifestyle for busy people with demanding schedules, that provides for increased energy, improved mood, and less anxiety and stress. I met with Joe along with other professional and executive colleagues of mine. Many of us have adopted his lifestyle recommendations, achieved positive results, and hold him in high regard.
Through the use of therapeutic interventions such as psychotherapy, healthy nutrition and aerobic exercise that reduce body fat percentage, and antidepressant medication, the destructive epigenetic processes may be reversed. As demonstrated in the picture below, these healing influences can activate so-called DNA “promoters” that enable the brain cell to code the RNA responsible for the production of neuroprotective proteins, resulting in increasing levels of these proteins. This restores normal cellular and mitochondrial energy functions, which in turn improve the information processing capabilities in multiple interacting circuits of the brain. This results in the normalization of emotional, cognitive and behavioral functioning.
These events are illustrated in the picture below. On the left hand side, the DNA is “promoted” to produce increased levels of BDNF. On the right hand side from top to bottom, in response to increased BDNF, the dendrites of the brain cells then regrow their branches, and the axons of the brain cells become re-enriched with dense packets of neurotransmitters. This restores and enhances healthy emotional functioning.
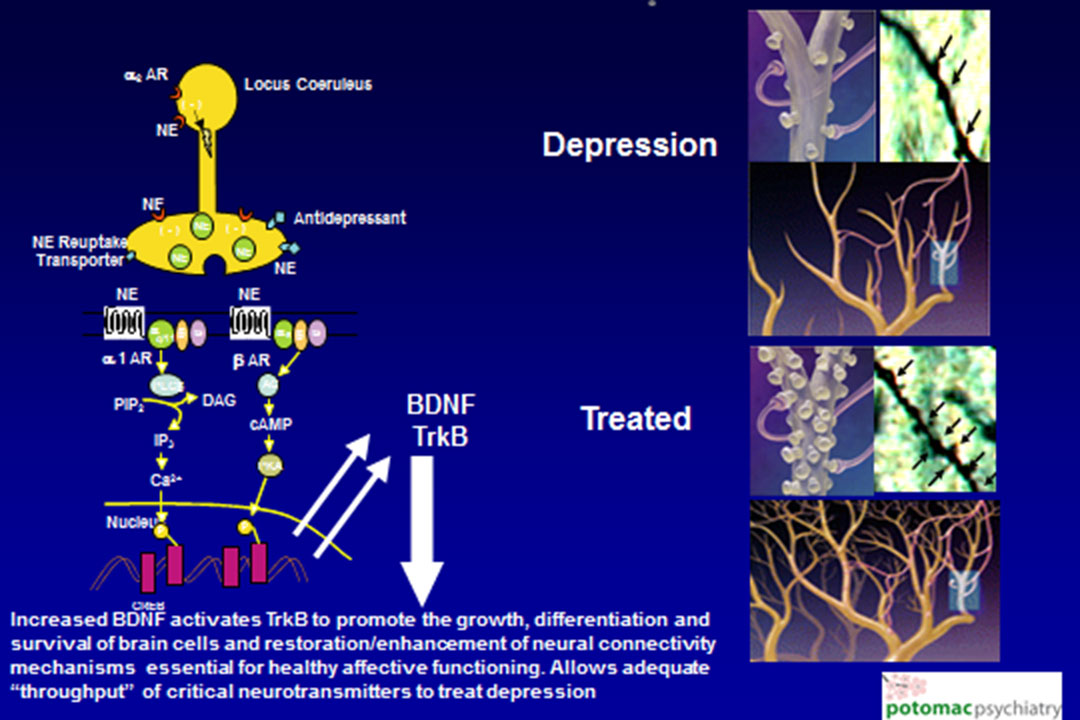
In viewing this process of regeneration, one can imagine that the implementation of psychotherapy, proper nutrition, and antidepressant medication is akin to the arrival of Spring, when tree limbs (and the human spirit) blossom, and experience a rebirth!
Related Information
- Learn about Genetic Testing
- Learn about Potomac Psychiatry
- Meet Our Doctors
- Contact Potomac Psychiatry
.png?width=144&height=144&name=Untitled%20design%20(34).png)


